A more personalised approach to breast cancer diagnosis and treatment
11 December 2019
Researchers at the Auckland Bioengineering Institute (ABI) and the Department of Engineering Science are combining machine learning and state-of-the-art imaging to develop an automated analysis technique that will radically improve the diagnosis and treatment of breast cancer.
The University of Auckland researchers, including Professors Martyn Nash and Poul Nielsen, and Dr Prasad Babarenda Gamage, have received $1.05 million in philanthropic funding to advance research in which they have developed biomechanical analysis techniques that automatically merges information from different medical images of the breast.
This will provide clinicians with more information about any abnormality, as suspicious lesions and warning signs for cancer can appear differently in the various types of images.
It can help, for instance, to co-locate abnormalities such as micro-calcifications – tiny and difficult-to-detect features visible on x-ray mammograms that can indicate early stages of breast cancer – with regions of increased blood supply identified using MRI and which can also indicate tumour growth.
One of the key issues with merging information from current medical imaging technologies is that they scan the breast in different positions.
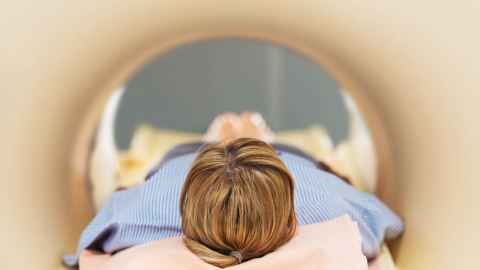
In an X-ray mammogram, the gold standard for the early detection of breast cancer, a patient is standing and the breast is compressed between two plates. If she is referred for ultrasound imaging, the image is taken while the patient lies on her back. In magnetic resonance imaging (MRI), the images are taken typically with the patient lying on her stomach.
As the breast is a soft organ that changes shape according to the position in which it is held, cancerous lesions can move around in response to the external loads. This can make it difficult for clinicians, surgeons and radiologists to identify the exact region that needs further investigation or treatment.
After a mammogram, follow-up imaging known as ‘second look ultrasound’ can involve clinicians spending up to an hour, just trying to find, with some degree of certainty, the same piece of abnormal tissue that they spotted on a mammogram.
“After a mammogram, follow-up imaging known as ‘second look ultrasound’ can involve clinicians spending up to an hour, just trying to find, with some degree of certainty, the same piece of abnormal tissue that they spotted on a mammogram,” explains Dr Nash.
“We're using biomechanics to predict the movements of those suspicious tissues, so when a person is lying on her back, such as during surgery, the surgeon can be provided with a much better idea as to where to find the suspicious lesion,” says Dr Babarenda Gamage.
“Most studies highlighted the difficulties in completely excising tumours in patients who underwent breast conserving therapy,” he says. “Incomplete excision means additional surgery to remove the remainder of the tumour, which increases the patient’s risk of infection, affects the cosmetic results of the surgery, and causes considerable psychological distress.”
Part of the challenge has been identifying the different biomechanical properties of the different types of breast tissues — to account for the individuality of each patient.
“Breasts come in all shapes and sizes”, notes Dr Nielsen, “and the mechanical properties of the tissues vary from person to person. So that provides a challenge: to create, realistically, individual specific models,” he says.
The team has been able to draw on 200 scans provided (with patient permission) by the Auckland District Health Board.
This success of their research can be attributed to a long collaboration with Dr Anthony Doyle, an MRI expert at Auckland City Hospital, who has worked with the team on identifying key clinical challenges that need solving and providing feedback on their research.
Dr Doyle says the researchers have made enormous progress in developing methods for analysis and mathematical modelling of breast tissue. “This work is approaching real-time clinical application, which is very exciting in terms of realising the benefits of advanced computational techniques in improving outcomes for patients.”
It has been a long-standing, close, and mutually beneficial collaboration, in which clinicians are learning more about mathematical modelling, and the bioengineering researchers are learning more about the real world challenges facing clinicians working with breast cancer. “If you’re working on clinical problems you need to have a close collaboration with a clinician,” says Dr Nielsen.
Media contact
Margo White I Media adviser
DDI 09 923 5504
Mob 021 926 408
Email margo.white@auckland.ac.nz