Helping babies born into nutritional emergencies
9 April 2021
Some babies are born into nutritional emergencies. Dr Barbara Cormack, of the Liggins Institute, explains why and what's being done about it.
When you’re starving, eating can be fatal.
'Refeeding syndrome’ was described after World War II, following liberation, when some chronically-starved Japanese soldiers died after they were fed a normal diet, because their bodies could not handle that amount of food.
Anyone with serious malnutrition, such as people with severe anorexia (nervosa), alcoholics or cancer patients, can be at risk of the biochemical disturbances known as refeeding syndrome, potentially causing infection, heart failure and death.
However, it’s only in the past decade that scientists began to suspect that very premature (preterm) babies might also be affected because they are born “malnourished” due to missing out on the nutritional stores usually transferred from the mother in the final months of pregnancy.
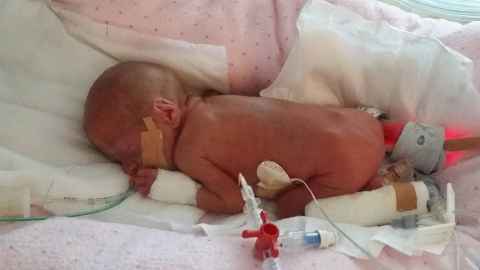
The smallest preterm babies weigh as little as 350 to 1000 grams, some small enough to fit in the palm of your hand. Now, research by the Liggins Institute has shown that refeeding syndrome can occur in very small preterm babies during the first week after birth and is associated with worse health outcomes.
Nutritional guidelines for neonatal intensive care units can standardise practices that vary from hospital to hospital and even within hospitals
Last year, the Liggins Institute completed the world’s biggest study of refeeding syndrome in babies with extremely low birth weights (under 1000 grams). We found an association between the condition and low levels of phosphate in the babies’ nutrition. Health outcomes were worst for babies in the hospitals that provided nutrition with the least phosphate.
This evidence of the importance of phosphate offers a way forward. Already, some hospitals in New Zealand and Australia have tweaked their feeding to make sure very preterm babies get more phosphate in the first week after birth. Hospitals have also begun routinely monitoring phosphate levels in babies over those early days.
And we’re expanding our research. One of my next projects is monitoring 100 extremely low birth weight babies in neonatal intensive care units in Auckland and Middlemore hospitals, to see if more phosphate can reduce the number of babies who develop refeeding syndrome.
Importantly, I also plan to lead the development of national nutritional guidelines for neonatal intensive care units, so that we can standardise practices that vary from hospital to hospital and even within hospitals.
You may be wondering: Why the big focus on phosphate? When a 'starved' baby receives nutrition, this increases the demand for phosphate by cells for energy production. If that nutrition does not have enough phosphate, levels of phosphate in the baby’s bloodstream fall, triggering an alarm in the body, which needs phosphate for a whole range of very important processes.

Going into emergency mode, the body starts dissolving its own bones. That process, called resorption, releases not only phosphate but also calcium, and can cause dangerously high levels of calcium in the bloodstream, a key factor in refeeding syndrome.
The Liggins Institute’s work on the condition is an offshoot of our ProVIDe trial involving 434 extremely low birthweight babies across six hospitals in New Zealand – Auckland, Middlemore, Dunedin, Christchurch, Wellington, and Waikato – and two in Australia, which is testing whether additional protein improves growth and neurodevelopment.
Seven years ago, around the time ProVIDe trial was set to begin, a scientific paper was published suggesting refeeding syndrome might occur in preterm babies. So, we added the topic to our study. We were surprised to find that 20 percent of the preterm babies we studied in New Zealand hospitals had refeeding syndrome.
Babies with the lowest phosphate levels in their blood were five times more likely to have a serious brain haemorrhage. They were more prone to infection, a serious concern in intensive care, and most importantly, the babies with refeeding syndrome were three times more likely to die before discharge from hospital.
Even before we have the primary outcome of the ProVIDe trial, this hugely valuable information will help us do much better for our most vulnerable babies by refining and standardising nutrition.
The Kelliher Charitable Trust is funding further research by Dr Cormack. She detailed her research at 'Survive to thrive: Feeding New Zealand’s preterm babies,’ a free public lecture and webinar which also featured Liggins Institute head Professor Frank Bloomfield, and paediatric dietitian Tanith Alexander.
Dr Barbara Cormack is a senior research fellow in the Liggins Institute.
Used with permission from Newsroom Born into a nutritional emergency 9 April 2021.
Media contact
Paul Panckhurst | media adviser
M: 022 032 8475
E: paul.panckhurst@auckland.ac.nz